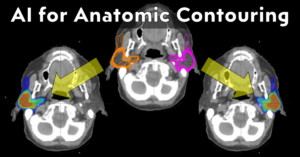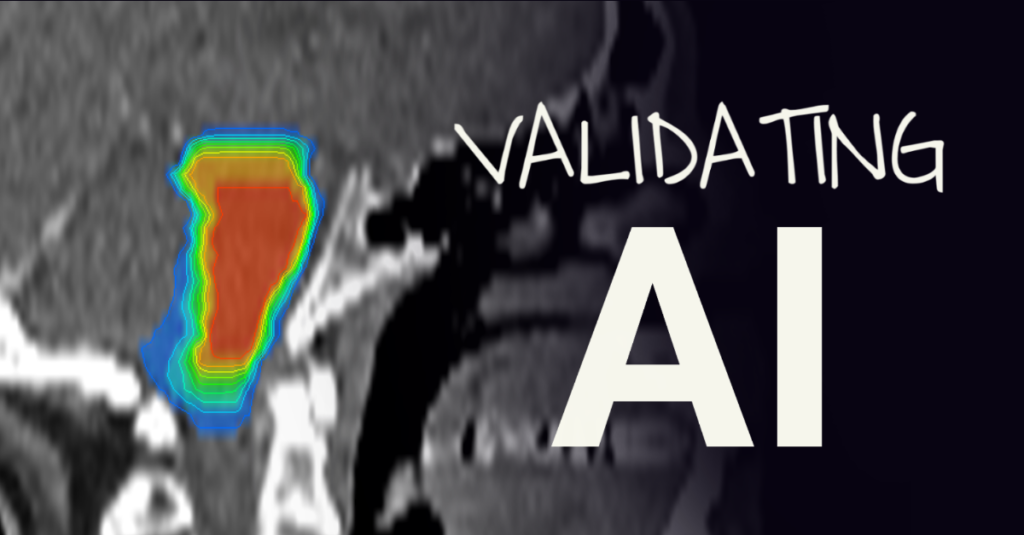
Dear AI Autosegmentation Vendors,
I am reaching out to any/all vendors to invite you to take part in periodic, non-funded podcasts. The forum will allow you to introduce yourselves, show your wares, and share your thoughts about how the radiation therapy industry can best validate AI autosegmentation engines/models.
The conversations will center around the imaging datasets and population of radiation oncologists’ manual segmentations that are generated by the non-commercial, not-for-profit project called “C3RO” (Contouring Collaborative for Consensus in Radiation Oncology).
Please see the details below. Email me (Ben Nelms) directly at canislupusllc@gmail.com if you are interested and would like to get on the schedule.
Thanks,
Ben Nelms
What
An unbiased podcast/interview series focusing on AI autosegmentation of human anatomy, specifically to use as an input to radiation treatment planning.
Why
Goal 1. Elevate the conversation about how best to validate AI outputs, both in the short and long term.
Goal 2. Get to know AI vendors in a casual, scientific, and “non-salesy” forum.
Goal 3. Show cool, real-time results from (1) populations of human experts and (2) AI engines.
Goal 4. Generate some pretty great ideas about how to build gold standards of human anatomy segmentation to use for both education of clinicians as well as validation of AI software.
Who
Host. Ben Nelms, Ph.D. (Canis Lupus LLC)
Guests. Representative(s) from any/all willing AI vendors and research groups who specialize in anatomy autosegmentation
Note: Conversations (likely all of them, or at least the initial ones) will be one vendor at a time. This helps ensure equal airtime and no distractions.
How
The conversation flow will be casual, with an underlying structure to cover some, if not all, of the following topics.
Intro. Your background, and what brought you to this field? (Optional) How does your group currently do validation of your AI outputs? Is it quantitative, qualitative, or both?(Required)
Data / Results. Generate contours – ideally in real time right before or in the early minutes of the meeting – for the imageset in question. Compare your automated outputs to (1) the population Isoagreement clouds and (2) various expert contours (if available), per structure....